What is it?
High digestive endoscopy, esophagogastroduodenoscopy or popularly known only as endoscopy, is an examination that allows visualization, through a camera, upper gastrointestinal tract, composed of esophagus, stomach and duoden (initial part of the small intestine).
Routing for the examination request is quite common when patients complain of pains in the region of stomach and beginning of the small intestine.
Although frightening most people, because it is a procedure that introduces the endoscope, endoscopy does not hurt and produces the minimum of possible discomfort, since it is made under sedation.
In addition, the exam is very complete, so its results are able to point out different directions from a possible disease, such as their location, category and also the degree of intensity.
In this article you will find the following information:
- What is it for?
- How is it done?
- Endoscopy hurts?
- When it should be made
- Contraindication
- Preparation
- Post-test effects
- Results
- What can affect results?
- Scratchs
- Price
- Complementary examinations
- Common questions
What is it for?
The examination is commonly requested to diagnose or treat diseases that achieve the high digestive system, which may present symptoms such as: persistent abdominal pain, nausea, vomiting and / or difficulty of swallowing.
This examination may also be required for the withdrawal of objects that may accidentally have been swallowed or can be used for the realization of esophageal mucosa biopsies, stomach or duodeno in order to detect diseases and conditions.
Therapeutic uses
Digestive endoscopy is also a widely explored procedure for therapeutic use in other diseases. It is considered a good method, because in addition to being minimally invasive, dispenses incisions in the abdominal region. Check out how it can be used:
- Intragastric balloon placement for obesity treatment;
- Placement of probes in patients with neglecting difficulty;
- Perform gastrostomy (surgical intervention for the placement of food probe);
- Withdrawal of polyps (polypectmies);
- Elastic ligature / sclerotherapy of esophageal varicose veins;
- Removal of foreign bodies (coins swallowed by children, for example);
- Treatment of bleeding lesions (ulcers, vascular lesions, tumors etc.);
- Dilation of stenosis (of the esophagus, stomach or duodenum).
How is it done?
Endoscopy is a very safe and simple examination, lasting 10 to 20 minutes. The exam consists of 2 small steps: the sedation and the introduction of the endoscope.
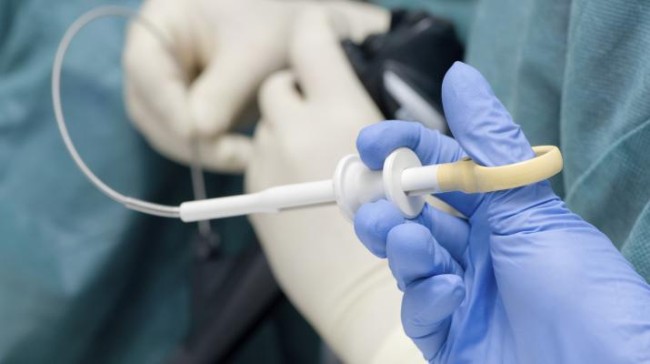
Sedation
In fact, sedation is a stage that precedes the procedure. As soon as the patient enters the examination room, he will be instructed to lie aside. In sequence a spray will be used in the throat in order to anesthetize the region, so the reflection of the vomiting is avoided.
Soon after, a short-term sedative is also applied, normally intravenously, so that the patient does not feel any kind of discomfort with the introduction of the endoscope.
Sedation has as main objective to prevent the patient from feeling pains and discomforts during the procedure.
For this to happen, two medications can be used: the midazolam or propofol. Both act on the central nervous system, more specifically in the activator reticular system, which is responsible for keeping us awake or sleeping.
Thus, they stimulate the sensation of drowsiness and sleep, besides, at the same time, also affect another region: the limbic system, which is responsible for the emotions.
In this way, sedation also stimulates the sense of well-being, being common for these feelings of relaxation when the patient wakes up.
Introduction of endoscope
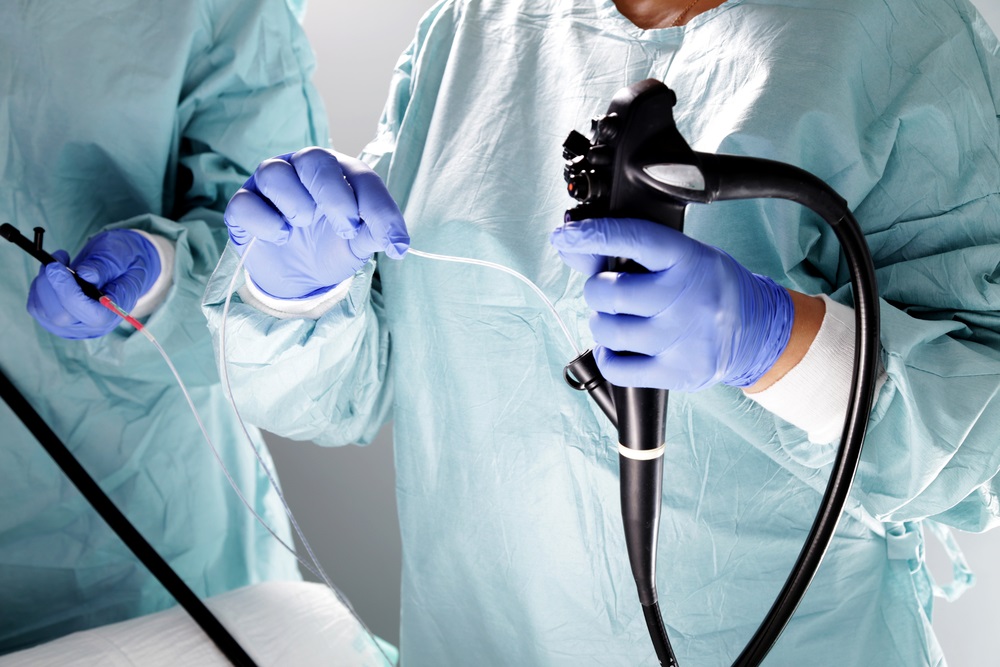
After the total sedation of the patient, which usually happens very quickly, the examination is actually initiated. The doctor, usually a gastroenterologist, introduces the tube, which is super flexible, by the mouth. The endoscope has a camera at its end, so soon after the introduction the doctor is already guided by the images.
Images recorded by the camera are transmitted in real time for a monitor that is next to the doctor, so the professional is not only guided, but also can already identify changes in the esophagus mucous membranes, stomach and duodenum.
In case of the doctor to find suspicious lesions, it is possible that a biopsy is realized, that is, small pieces of mucosa will be removed in a totally painless process so that a pathologist can be able to evaluate the sample in the sequence.
Along the examination, bloody lesions can also be found. If this is the case, the professional can cauterize the location for bleeding to be contained. In the examination, it is still possible to withdraw objects that have been accidentally swallowed.
During the procedure, it is also common for the introduction of air. She will be responsible for “detaching” the walls of the organs that are very joining and thus facilitates the internal visualization. This introduction of air is done by the endoscope, which already has such a mechanism.
Endoscopy hurts?
Because it is an examination that is performed under sedation, endoscopy does not hurt. The patient may feel a slight discomfort in the throat after the procedure, but that must pass soon in the early hours.
When it should be made
This type of examination is usually requested by the gastroenterologist after the patient complaining of stomach pain, difficulty or pain to swallow, burning, vomiting or any discomforts in regions where the organs of the digestive system are located.
Its achievement can help identify the motives of symptoms without defined cause, including persistent heartburn, difficulty of swallowing and bleeding.
In addition, the examination may also be requested for people who have a history of stomach cancer in the family or conditions that provide the appearance of the disease.
The procedure may still be required to detect the presence of H. pylori bacterium, although there are other less invasive methods that can confirm or not suspect.
In addition to those already mentioned, there are also other reasons for which it is indicated that, although fewer recurring, are equally common as others:
- Investigate painframes of pain or unexplained discomfort in the upper abdomen;
- Evaluate the severity of the gastroesophageal reflux disease, which does not respond to the initial clinical treatment;
- Trace cancer in patients with prior diagnosis of Barrett esophagus;
- Investigate persistent nausea and vomiting.
- Evaluate and possibly treat top gastrointestinal tract bleeding frames (such as vomiting with blood or digested blood signs, suggesting the stomach as cause);
- Investigate esophageal varices in patients with cirrhosis and / or portal hypertension;
- Investigate cadres of anemia for iron shortage without defined cause;
- Investigate frameworks of difficulty swallowing food or sensation of eating food in the esophagus;
- Remove an accidentally swallowed foreign body;
- Investigate weight loss without apparent reason;
- Investigate the patient’s possibility to possess celiac intolerance;
- Evaluate gravity of the esophagus lesion in patients who ingested caustic soda, sanitary water (bleach) or any other corrosive substance;
- Evaluate cure or evolution of polyps, tumors or ulcers found in previous endoscopies.
Contraindication
There is no contraindication for performing the examinations. However, patients who have respiratory, neurological or cardiac problems must inform their doctors.
In addition, patients with a history of medications allergy should also be attentive and inform the health professional.
Preparation
The main recommendation that should be followed before the examination is not to feed in 4 to 8 hours preceding the time of the procedure.
Thus, the stomach will be empty, avoiding the patient vomite. This also facilitates the vision of the doctor without the presence of food remains.
For patients who use continuous drugs, it is always important to inform the laboratory and clinic where the exam will be taken at the same time as the appointment. Check out these medicines:
- Aspirin or those who have aspirin in their composition;
- Medications for arthritis and diabetes;
- Blood pressure regulators;
- Blood thinners;
- Anti-inflammatory drugs such as ibuprofen.
This way they will know or tell if there will be no need to change the administration of the drug.
It is also not recommended that the patient make intake of antacids, as they are able to change the pH of the stomach, which can interfere with test results.
In addition, the presence of a companion is essential for the exam, even he shall only be initiated at the time the other person is on site.
This requirement is because the sedative used in the procedure may cause some effects.
Post-test effects
As one of the steps taken is sedation, most of the post-exam sensations relate to it.
Upon completion of the procedure, usually the patient waits between 20 and 30 minutes in a room until he wakes up and the effects of sedation are already more mitigated.
Once the patient awake, a slight feeling of tiredness or lack of concentration can be felt. Both are feelings that will be mitigated as time goes on.
It is also common to have total amnesia regarding the examination, including patients often do not believe they have already undergone the procedure.
Despite the effects of anesthesia are light, medication may still continue taking effect for up to 8 hours. Therefore, after examining the person is not able to drive, work, or make important decisions.
Some feelings can still manifest after the analgesic effect of end spray, as a mild sore throat. Some patients also experience abdominal distension, air result that may have been introduced during the examination.
There are other directions that are normal after the following:
- Wait for the anesthesia at the site where the procedure was done for a time which can vary from 30 minutes to 2 hours or as the physician deems necessary;
- Rest at home after the examination;
Symptoms such as discomfort or vomiting in the hours that follow endoscopy are also relatively common.
Results
As upper endoscopy is a test that analyzes three bodies, there are many possibilities results. However, the most common request is from gastritis suspicions.
Sometimes, the results of the procedure can be taken immediately, even though the official report take a few days to be released, especially those who need biopsy.
The results have always three parameters established by the Sydney System: topography, category and level of intensity.
Topography
This parameter focuses on point at which the stomach region gastritis is affecting:
- Pangastritis: gastritis is spread throughout the esômago;
- Den gastritis: gastritis is located only in the antrum (final part of the stomach);
- Gastritis of the body: gastritis is located in the central region of the stomach.
Category
There are seven categories of gastritis, which relate to the type of injury that it causes:
- Enanthematous: presence of red rashes in the region where gastritis is located;
- Erosive: There mucosal erosions and may be flat or raised. Usually prior to formation of ulcers;
- Atrophic: chronic inflammation of the stomach mucosa, resulting in the loss of cells forming the glands that produce gastric juice. Thus, there is a substitution of stomach cells by intestinal cells;
- Hemorrhagic: there is bleeding in the stomach, and the patient also has symptoms like vomiting of blood, black stools, pressure drop and paleness;
- Reflux (reflux or alkaline bile reflux): reflux of duodenal reaches the stomach, causing a chronic mucosal injury;
- Hyperplastic: significant increase in the number of cells in any layer of the stomach, resulting in an enlargement or height greater gastric folds. It is usually associated with other diseases such as Ménétrier disease or Zollinger-Ellison syndrome.
Degree of intensity
On examination, which is still on the level of intensity of your gastritis:
- Light;
- Moderate;
- Severe.
This nomenclature indicates at what stage the disease is or how long it is installed in your body.
What can affect results?
At first, there is no medicine that can affect the results of the endoscopy examination.
What will be critical to a clear exam result is how it was done. The professional needs to be well attentive to the images to not miss any different texture or coloring, for example.
It is worth remembering that the examination should always be done by a gastroenterologist or an endoscopy, as these professionals are those skilled for both the examination and the understanding of the images captured by the endoscope.
Scratchs
Endoscopy is considered extremely safe examination, having minimal risks. Symptoms that may indicate a problem include fever, difficulty swallowing, chest pain or abdomen and vomiting. Among the possibilities of complications are:
Reaction to sedatives
If you make use of any constant medication or is allergic to some medicine, it is always important to inform your doctor or when you are marking the exam.
It is also important to inform you if you have a disease that entails respiratory, cardiac or neurological problems.
Some possible effects caused by sedatives are:
- Difficulty breathing;
- Excessive perspiration;
- Low blood pressure;
- Slow heart beat (bradycardia);
- Spasm of the larynx.
Bleeding and drilling
There is still a minimum risk of bleeding when a biopsy is needed during the examination.
There are also a few cases of drilling of the esophagus, stomach or duodenum, which should be treated with the patient’s hospitalization.
Infections
There is a patient’s risk to contract infections during the procedure. In general, the possibility is minimal and the infection can be treated with the administration of antibiotics.
Price
The high digestive endoscopy exam is available for both SUS and by most health plans. The price of the exam in private clinics may vary between 150 and 200 reais.
Some places have a different price when the biopsy needs to be made.
Complementary examinations
In addition to high digestive endoscopy that, as already mentioned, is restricted to high digestive tract care, there are other examinations that also investigate diseases located in the digestive system:
Colonoscopy
Colonoscopy is the examination characterized by the observation of other organs of the digestive system, such as the final part of the small intestine and all the large intestine. Because of this, it is also considered an examination of digestive endoscopy.
In the same way that endoscopy, colonoscopy occurs with the patient sedated, but the introduction of the flexible hose, which in this case is the colonoscope, occurs through the anus.
Endoscopic ultrasound
This examination is requested for investigation of diseases on the walls of the stomach, in the near tissues and lymph nodes.
Often, endoscopy is a part of the endoscopic ultrasound exam, which is characterized by the use of sound waves capable of producing real-time images.
Inscribe
Enteroscopy is an examination used for the investigation of diseases of the gastrointestinal tract, mainly of the small intestine. In it, a enteroscope is used and there is a collection of fragments of the mucosa.
Common questions
Can pregnant women do endoscopy?
Although the exam, itself does not bring any risk to the pregnant woman or the baby, endoscopy should only be accomplished if there are suspected diseases that threaten the life of the pregnant woman or promote much discomfort.
This is because the medication used for sedation can cause poor training in the fetus, especially in the first 3 months, in which neural tube formation occurs. It can also promote the interruption of gestation.
I have diabetes, can I use insulin on the exam day?
You will probably have to adapt the dosage of your insulin on the day of the exam. In any case, it is important to inform the situation for the doctor, so it may judge the need to adjust your dose and how it should be administered.
Can I go back driving on the exam day?
Not at all. As already commented above, the exam will only be carried out with the presence of an escort, since the effects of anesthesia may leave the patient disoriented.
For the same reason, it is not recommended that the patient directs, for he may not be with all his reflexes clear enough.
It is also not recommended to operate machines or other types of jobs.
Why do not I remember the examination?
Amnesia in relation to the endoscopy examination is a fairly common effect, result of using sedation used during the procedure. The absence of remembrance by the patient is an indication that the procedure was performed without pain or discomfort, so amnesia is desirable.
This loss of memory should extend for a maximum one hour. Even if the patient wakes up shortly after the end of the procedure, which usually last 30 minutes, he will also not remember the moment that will be under observation while the effect of anesthesia passes.







